Recovery in Motion – A Comprehensive Breast Cancer Recovery Program
Breast cancer treatment and surgery can affect the body, particularly the affected side, in various ways. Part of making a full recovery is being aware of these changes and takings steps to recover fully.
Before Surgery
It is a good idea to have an assessment with a certified lymphedema therapist before your surgery in order to take measurements of both your arms. Patients who have lymph nodes removed and/or radiation therapy, are at increased risk of lymphedema. Lymphedema is a form of chronic swelling in the arm or chest area that affects approximately 18% of breast cancer patients. This is discussed more fully further down.
After Surgery
After surgery you may experience pain and stiffness around your incision in the chest, armpit, shoulder and/or abdomen. Numbness and tingling is sometimes noted near the incision area and the inside/back part of your upper arm, from the armpit to the elbow. The intensity of these symptoms may vary. However, they usually improve or disappear over time as you heal and become more active. Because nerve endings grow slowly, it may take six months to a year to regain normal sensation.
Immediately after surgery mild to moderate pain is common. To regain functional use of your arm, it’s necessary to use your hand and arm as normally as possible. Resist the natural impulse to protect your arm by holding it close to your body. This will help to promote good posture and circulation and help to prevent muscle and soft tissue tightness from developing in the chest, underarm and shoulder.
Activities
You may have temporary restrictions and limitations in your arm movement after
surgery. This can affect your normal activities. Initially for the first two
weeks, and especially while the drain is in place, do not raise your elbow
above your shoulder level. Typically the drain under your arm is removed in 7-10 days after surgery. Whether you have had a lumpectomy, mastectomy or reconstruction, you should wait for two weeks before lifting your arm above 90 degrees (shoulder height) to allow the tissue to heal. After two weeks, you are encouraged to move the arm overhead with self-care activities.
The activity guide and exercise program to follow will be helpful in regaining maximal shoulder movement after surgery.
Activities you may do immediately after surgery include simple tasks such as:
- Washing
- Dressing with care i.e. button up tops
- Feeding yourself
- Showering (no baths).
It is important to listen to your body and not to overdo it. Remember to balance rest with activity. Any increasing pain should be discussed with your doctor or therapist.
Once the drains are removed you should begin to increase your activity and arm movement by:
- Washing and brushing your hair
- Dressing normally
- Hanging clothes in the closet
- Taking light weight dishes or goods in and out of the cupboard
- Dusting
- Light household
chores - Brisk walking for 10-30 minutes daily (when walking, allow your arm to swing freely)
Avoid:
- Pushing
- Pulling
- Heavy Lifting (anything above 2kg)
- Driving
- Swimming
Support your arm by:
- Do rest your arm on a pillow next to you or on your lap when seated.
- Do rest your arm on a pillow when lying on your side or on your back
- Don’t hang your arm over the side of the bed when sleeping.
- Don’t hold your arm tight against your body when seated or standing. This will cause shoulder strain.
- Don’t allow your arms to hang by your sides when seated.

Scar Tissue Management
As your incision heals, scar tissue may cause tightening under the arm and around the incision. You can begin scar massage when the drains are removed and the incision is completely closed with no drainage. This is usually 2-3 weeks
after surgery. (If you have reconstruction, check with your doctor first before
beginning scar massage.)
This gentle massage helps to keep the skin soft and supple and lowers the risk of
post-surgical pain.
How to Massage: Using the pads of two fingers, apply gentle pressure to the incision line and make small circular movements. Only do this massage for 4-5 minutes a day, so as not to irritate the healing skin. This daily massage should be continued until you can comfortably move and raise the arm without any feeling of tightness and pulling over the operation site.
Lymph Node Dissection
To determine if the cancer has spread beyond the breast area, your surgeon may perform a sentinel lymph node dissection (SLND) or an axillary lymph node dissection (ALND).
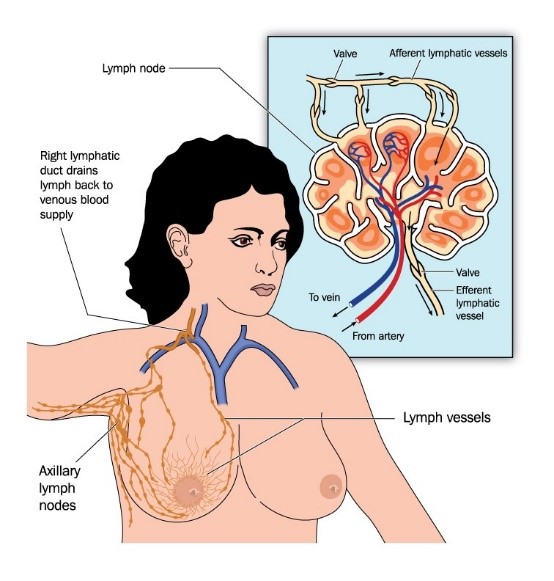
The lymphatic system is made up of lymph nodes and vessels that carry water, white blood cells and other important substances through the body. Lymph nodes act as filters and help to fight infection. Removal of lymph nodes may
cause a disruption of fluid flowing in the vessels. This could lead to fluid build-up (known as lymphedema) in the arm, hand or chest. Generally, the more lymph nodes that are removed, the greater the risk of developing lymphedema. There is a genetic pre-disposition to lymphedema too.
Having radiation therapy can also add to the risk for developing lymphedema.
If you have axillary lymph node dissection, lymphedema can develop in the arm, chest, back or breast, months to years after surgery.
Anyone who has had lymph nodes removed has a lifetime risk of developing lymphedema in the region where the lymph nodes were removed.
When lymph nodes are removed, the lymphatic fluid can slowly build-up, making it harder for the area involved to manage the accumulation of fluid. The build-up of this lymphatic fluid can increase the risk of skin infection.
Remember that lymphedema is a slow build-up of fluid. If you have sudden swelling in your arm – contact your doctor urgently. You should take special care of your arm to prevent injury or infection while still using your arm as normally as possible.
Signs to watch out for are:
- Slowly progressing swelling during the day
- Clothes and/or jewellery feeling tight
- Fullness and heaviness to the arm
- Skin infection
Lowering Your Risk of Lymphedema
A great deal can be done to prevent the onset or triggering of lymphedema. Remember that lymphedema can be triggered years after surgery so the following recommendations should become a lifelong practice.
- Do not allow injections, IV lines or blood samples to take place on the affected arm. You have the right to say ‘no’ and request that the opposite arm is used.
- Do not allow your blood pressure to be taken on the affected arm. Request that the opposite arm is used.
- Do not wear any tight, elasticated clothes, sleeves, or jewelry on the affected arm. Swap your ring to the other hand.
- Try to avoid carrying heavy items with the affected arm.
- Monitor the arm and check measurements annually if you have any concern.
- Skin hygiene and care.
Axillary Web Syndrome or Cording
Cording is inflammation and scarring of the lymphatic vessels and veins that sometimes occurs after breast cancer surgery, lymph node dissection and/or radiation. You may notice tight, string like bands of tissue pulling in the armpit and sometimes radiating down the arm and up the neck. Although painful and restrictive, they are not dangerous and usually resolve by themselves over time.
Physical therapy and massage can help to speed up recovery from cording. Contact your lymphedema therapist should you feel any pain or pulling in the area.
Maintaining a Healthy Weight
Being overweight or gaining weight after surgery places you at higher risk of developing lymphedema. While we don’t recommend any specific diet, a healthy lifestyle is recommended.
- Reduce or cut out the intake of sugar, especially sugary cool drinks and fizzy drinks.
- Moderate portions of white bread, pasta and rice.
- Reduce the intake of processed meats such a salami, ham etc
- Focus on eating vegetables, fruit and protein such as fish or chicken.
- Introduce nuts and seeds into your diet.
- Visit your doctor to check your D3 and B12 vitamin levels.
- Walk a minimum of 30 minutes a day. Even if you feel tired, make this a
daily routine. - 7-8 hours of sleep per night.
- Drink 2 litres of water daily.
Exercise and Movement
The importance of walking daily cannot be over emphasized. It can be difficult due to fatigue but it has in fact been proven to help with the lack of energy and tiredness that you might feel after surgery. Aim to walk for 30 minutes daily.
The lymphatic system does not have the heart to pump fluid around the body. It relies on the movement of the body (muscle pump) to work. Gentle stretching
exercises such as yoga and strength exercises such as Pilates are ideal to stimulate lymphatic flow and help in your recovery.
Swimming is an excellent form of exercise.
Our aim is to assist you to recover fully and to resume the activities and sports that you love to do. Speak to your therapist about which activities you enjoy.
Setting goals can be a very positive part of your recovery.
All activities should be cleared with your doctor before commencing.
Exercise Program (Download Exercise Program here) –> Recovery in Motion Exercises Phase 1 and 2
The following exercise program is designed to help you regain the full of your arm after surgery. There are two levels of exercise:
- Phase 1 exercises are to be performed beginning the day after surgery. An important note on these exercises is that you do not lift your elbows past shoulder height for these exercises. All patients do these exercises for the
first 2 weeks. - Phase 2 exercises are to be performed after 2 weeks for all patients (and your drain must be removed). At this point, you are to work hard to raise your arm fully over your head in different positions.
You should continue to exercise until you have regained the full use of your
arm. For most people, this occurs within six to eight weeks. After you have gained full movement of your arm, we recommend that you stretch at least once or twice daily for the first year to maintain your movement.
When performing your exercises, you may experience a mild degree of discomfort.
- Feeling a slight to moderate stretch during arm movement is normal.
- Feeling a sharp pain during or after exercise is not normal.
- Slight pain in your shoulder for ½ to 1 hour after exercise is normal.
You can avoid increasing the amount of discomfort you experience by:
- Performing all arm motions slowly.
- Using extra caution if you are on a strong pain medication as your sensation to pain may be altered.
- Reduce the number of repetitions or the intensity of your movement if soreness lasts more than 1 hour.
Phase 1 (Week 1 & 2)
Exercise 3 times daily, starting with 3 repetitions at each session, and add 1 repetition each day until you are doing 10 repetitions for each exercise.
With these exercises, you will get the best effect by moving to the position described and holding the stretch for a slow count of 5 seconds. Follow the prescription below.
Phase 2 (Week 3 onwards)
- You should continue to do any Phase 1 exercises that you find helpful.
- Begin with short daily walks around the house.
- Progress your activity as tolerated.
- You can safely return to most exercise by 6 weeks after your surgery depending on the type of surgery you had. (discuss this with your surgeon and therapist)
Follow Up
It is a good idea to have regular check ups with your therapist for the first 6-8 months after surgery. With appropriate exercise, scar tissue management and manual lymphatic drainage, you should aim to have normal range of motion in the shoulder, soft and movable tissue over the operation site and know that your arm measurements are remaining stable. Any signs of swelling to the arm, chest or back should be reported right away.