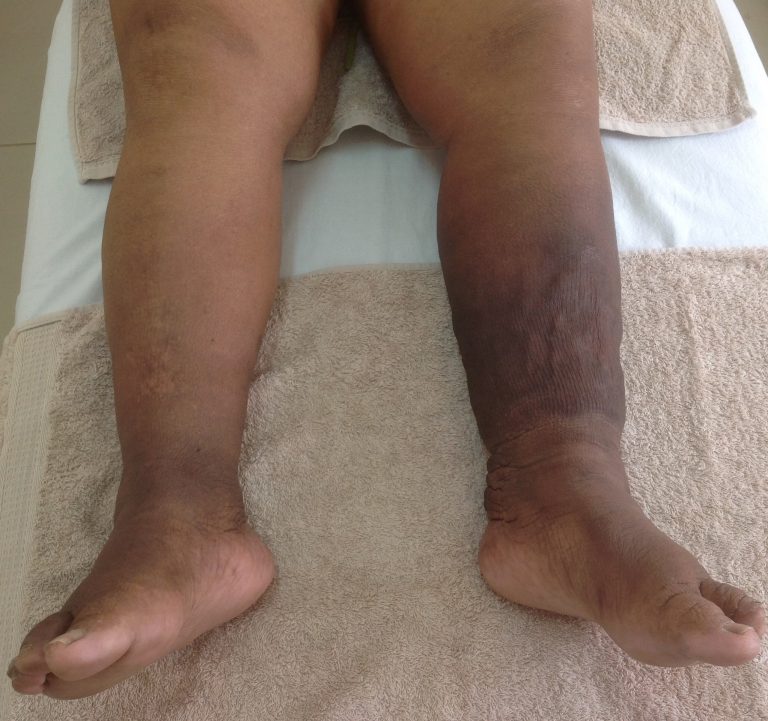
Phlebolymphedema
Phlebolymphedema is a combination of venous insufficiency and lymphatic insufficiency. It is most commonly due to the inability of the lymphatic system to adequately drain the interstitial fluid that accumulates in severe chronic venous hypertension. In a nutshell, patients who have a problem with varicose veins and poor blood circulation often develop a problem with swelling in the lower leg. And this is due to the lymphatic systems inability to cope.
The lymphatic and blood circulatory system together form the circulatory system of the body. They work closely together and it stands to reason that should one system be ailing, the other will be affected.
Patients with long term, poorly managed varicose or venous problems often go on to develop a degree of chronic swelling. And likewise, poorly managed lymphedema has a detrimental effect on the blood circulatory system.
When diagnosing phlebolymphedema, the therapist will be looking for the tell tale sign of hemosideran staining of the skin and itching in combination with the classic signs of lymphedema such a pitting, fibrosis and textural changes to the skin.
The dark change in colour to the skin is often the first visible sign of circulatory problems. One of the first questions patients ask once starting treatment is whether or not the colour of the skin will return to normal. Unfortunately the stain to the skin might improve a little as the texture of the skin responds to treatment but it can never return to normal. It is the pigment in the blood that causes this permanent stain to the skin in the affected area.
Another symptom of circulatory problems is the loss of normal body hair to the lower leg. The therapist will take note of all these signs and symptoms and check for good blood flow into the leg before giving a diagnosis and starting compression therapy.
Mild cases of Phlebolymphedema are able to be treated right away with compression stockings. Usually the knee high stocking is sufficient. For patients with varicose veins that extend further up the leg, the thigh high stocking is needed. Patients will be advised to wear the stockings for all the hours that they are upright and to sleep without compression. These medically graduated stockings will have the dual benefit of pushing blood efficiently back up to the heart and of helping the lymphatic system to drain all excess fluid out of the lower leg. Patients can start to feel the benefit within 24 hours of use.
More advanced cases where there are changes to skin, wounds and fibrosis, will need an intensive phase of therapy (Complete Decongestive Therapy) whereby a compression bandage is worn for a number of days in order to reduce the swelling and heal the skin. During this time, the patient is taught how to self bandage so that they have this skill for life in order to manage better at home. Once the swelling is reduced and the skin is healed the patient will be fitted with compression garments to wear during the day. It is common for the more advanced cases to need to self bandage at night for life to avoid recurrence and have proper management over Phlebolymphedema.
It is so important for patients to keep up to date with the regular replacement of their compression garments. Stockings that are worn daily need to be replace every 3-6 months and bandages replaced every 8-12 months. Once the fibres in the garments start to lose their form, the effectiveness reduces. Juzo compression is top quality in terms of the materials used and mode of manufacture which means that they last longer.
Lipolymphedema is diagnosed in patients with lipedema that, without treatment, has negatively impacted the lymphatic circulation in the legs. Lipedema is a fat disorder characterised by abnormal fatty tissue from hip to ankle. The foot is not affected. Once lipedema patients start to experience swelling in the feet and toes we can assume that the lymphatic system has been impacted and that lymphatic insufficiency is present.