Conditions Treated with Compression Therapy
Lymphedema
Lymphedema is a protein rich swelling or collection of fluid usually affecting the arms or legs. It can also affect the abdomen, chest, back, groin and head/neck. The area affected depends on where the lymphatic system is damaged.
The lymphatic system forms part of the circulatory system. A complex network of vessels and nodes drain the fluid from the tissues and organs and transport it to the subclavian vein where is re-enters the blood circulatory system. It is also an integral part of our immune system.
When this drainage and immune system is damaged, chronic swelling or lymphedema can develop. Patients with lymphedema can suffer repeated bouts of cellulitis skin infection in the affected area due to lowered immune response.
Primary lymphedema is a genetic condition that can be evident from birth (Milroys Disease) or it can manifest later in life; at puberty (Meige disease) or at age 35+ (Lymphedema Tarda).
Secondary Lymphedema is more common and is due to damage or trauma to the lymphatic system. A mosquito borne infection, Filariasis, causes the largest number of lymphedema cases in endemic regions. In the developed world, cancer treatments such a lymph node removal and radiation therapy cause the majority of cases.
Stage 0 – latency phase with no visible swelling. Sub clinical symptoms only.
Stage 1 – Visible swelling that spontaneously reduces with elevation of the affect area.
Stage 2 – Visible swelling that no longer spontaneously reduces.
Stage 3 – Visible swelling with skin changes, fibrosis and papillomatosis.

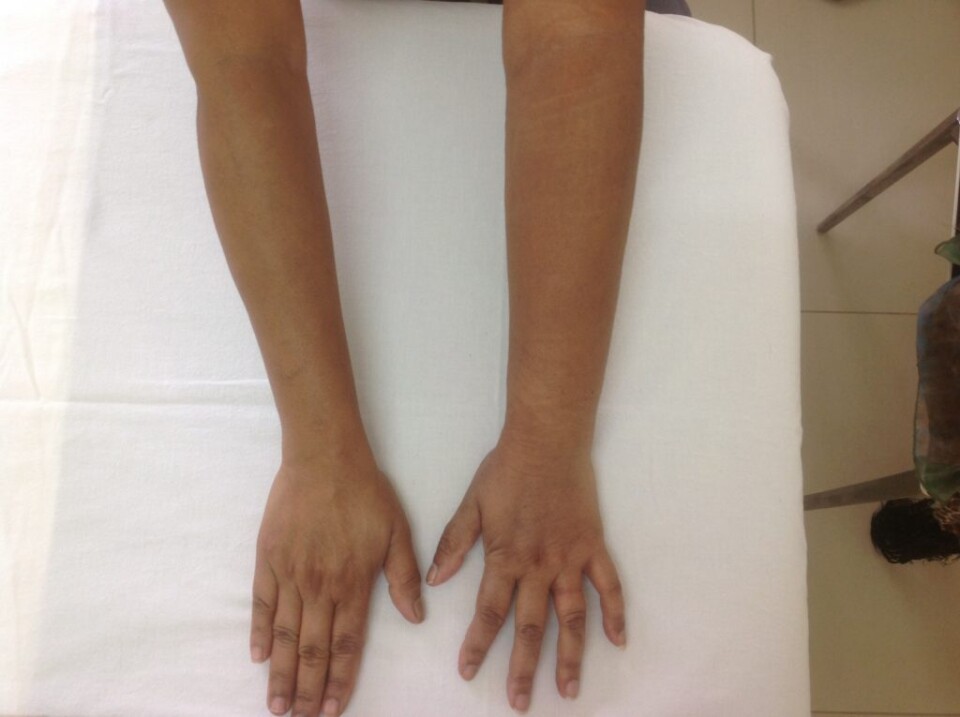
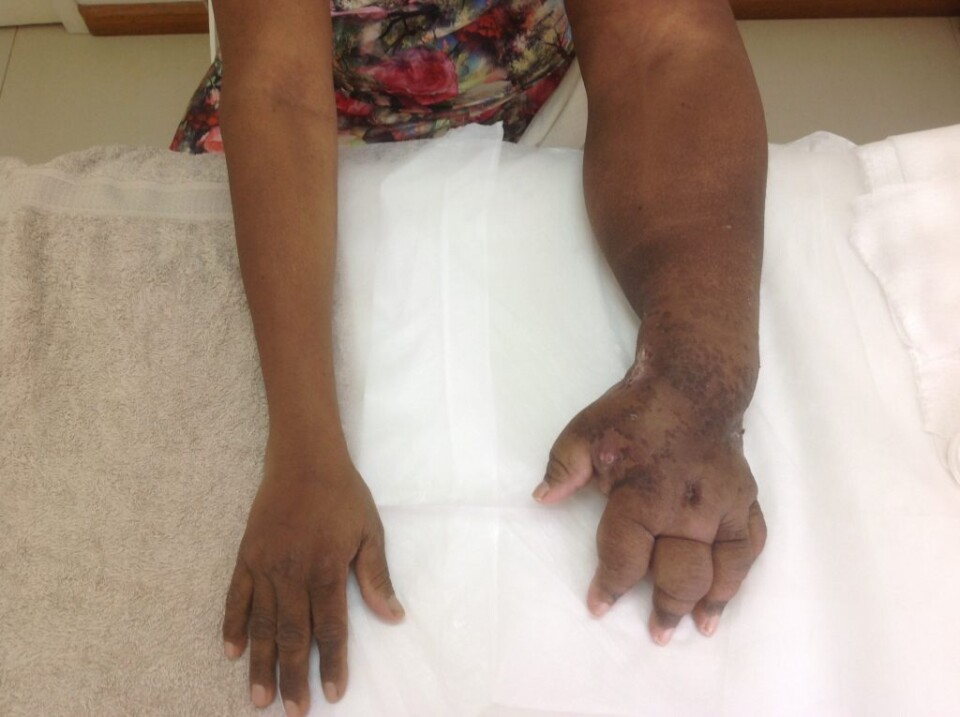
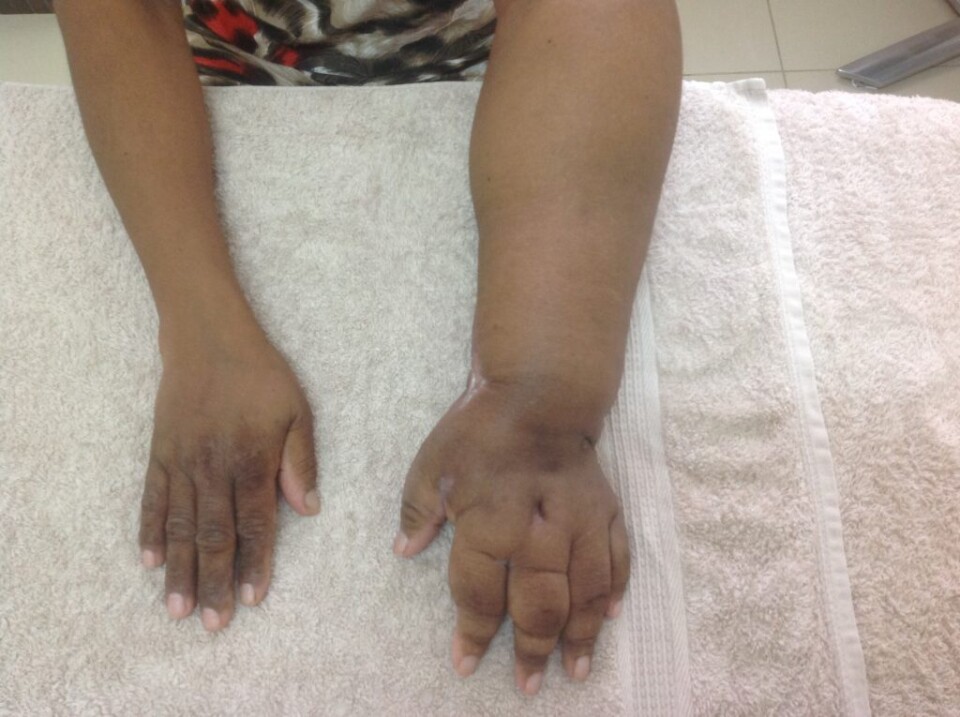

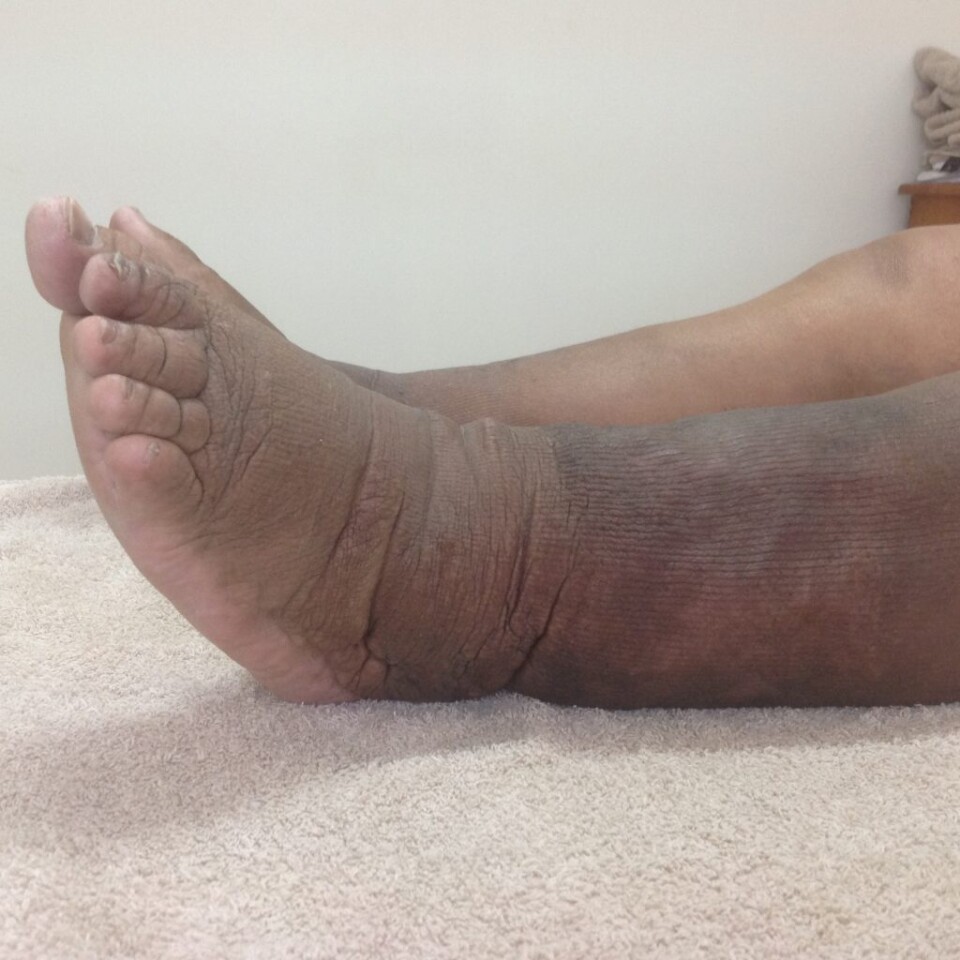
Phlebolymphedema
Phlebolymphedema is a combined insufficiency of both the venous (blood circulatory) and lymphatic systems. It is characterised by swelling, skin changes and skin discolouration. It is found predominantly in the lower extremity.
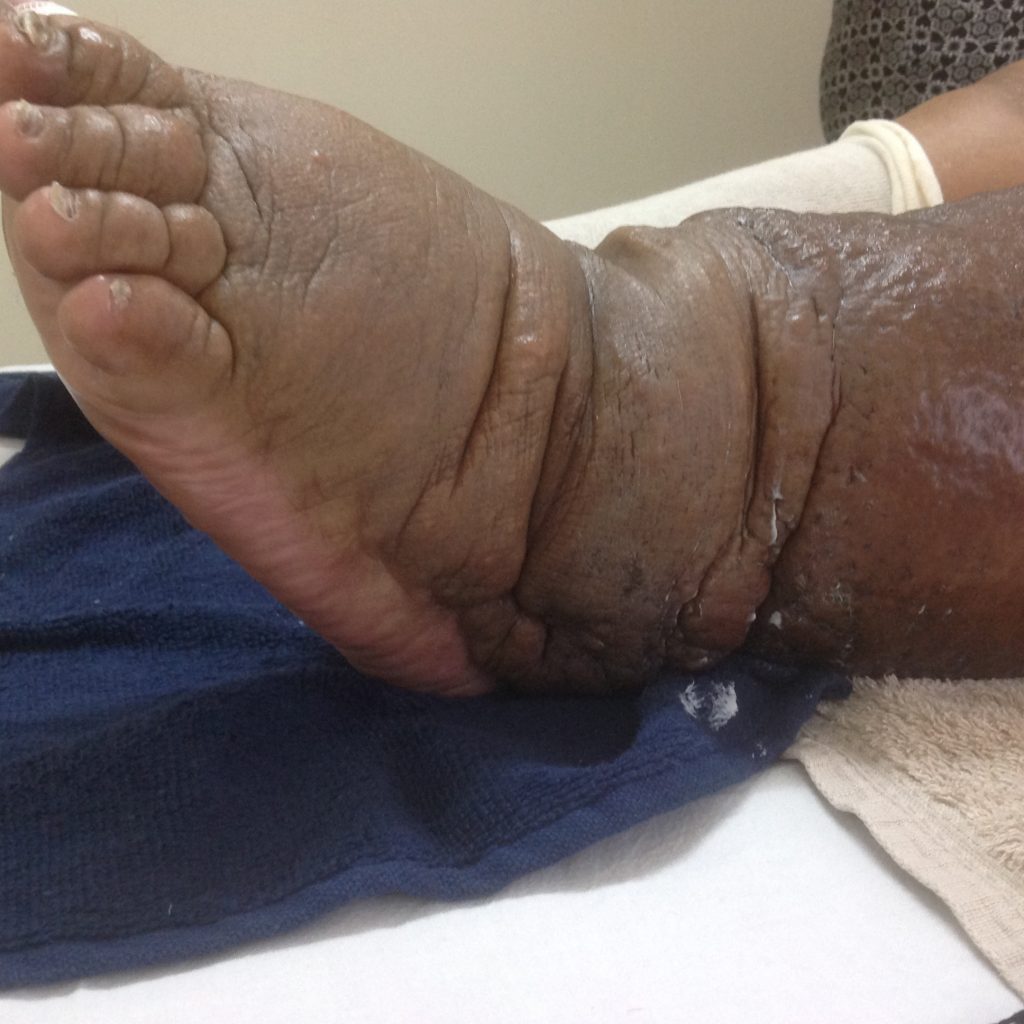
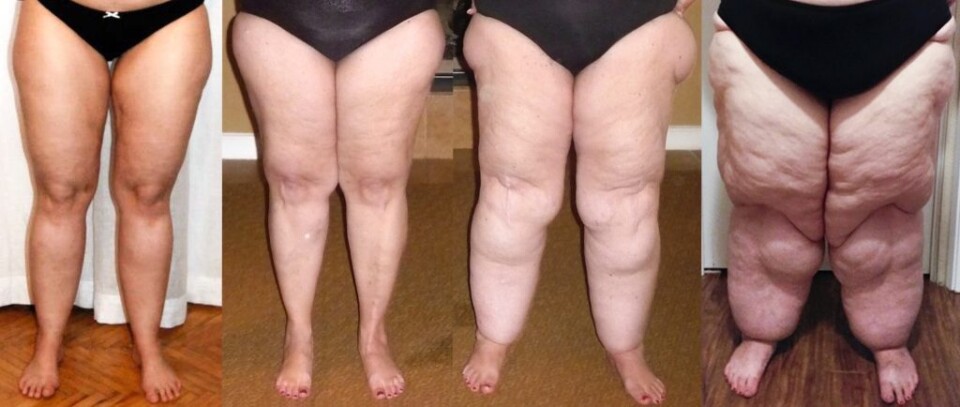
Lipedema
Lipedema has very recently been recognised as a medical condition. Women with lipedema have for years been told they are fat and need to diet and exercise in order to manage the fat distributed on their hips and legs. We now understand that no amount of dieting or exercise will shift the fat cells that create the condition now known as lipedema.
Some key symptoms of lipedema patients:
Treatment for lipedema is geared around compression and healthy lifestyle. Even though diet does not directly improve the lipedema itself, weight management and fitness are very important. Good muscle tone and overall fitness are crucial.
Ideally compression in the form of ankle-waist stockings should be worn daily. This gives an external compression that assists with lymphatic flow and slows progression. Stockings also contain the fat and give the legs shape making it easier for the patient to choose clothing and to exercise.
It is difficult to get lipedema patients to accept compression in the early stages. Once a patients mobility and psycho-social outlook is affected by lipedema they are more open to the benefits of compression. In fact, most patients love their compression once they feel the difference.
Venous Ulcer
Venous ulcers are wounds usually found on the lower leg due to venous disease. Improper functioning of the valves stop the adequate return of blood to the heart resulting in venous hypertension, skin changes, acute and chronic wounds. In order to gain wound closure it is necessary apply compression to the lower leg so as to exert pressure on the veins and increase the pump action of the calf muscle.
Moist wound care protocols combined with compression therapy have a profound effect on wound healing.
What do all these conditions have in common? They all respond well to compression therapy.